prime therapeutics prior authorization form pdf

prime therapeutics prior authorization form pdf

Prime Therapeutics Prior Authorization Form Fill Online

prime therapeutics prior authorization form pdf
prime therapeutics prior authorization form Archives
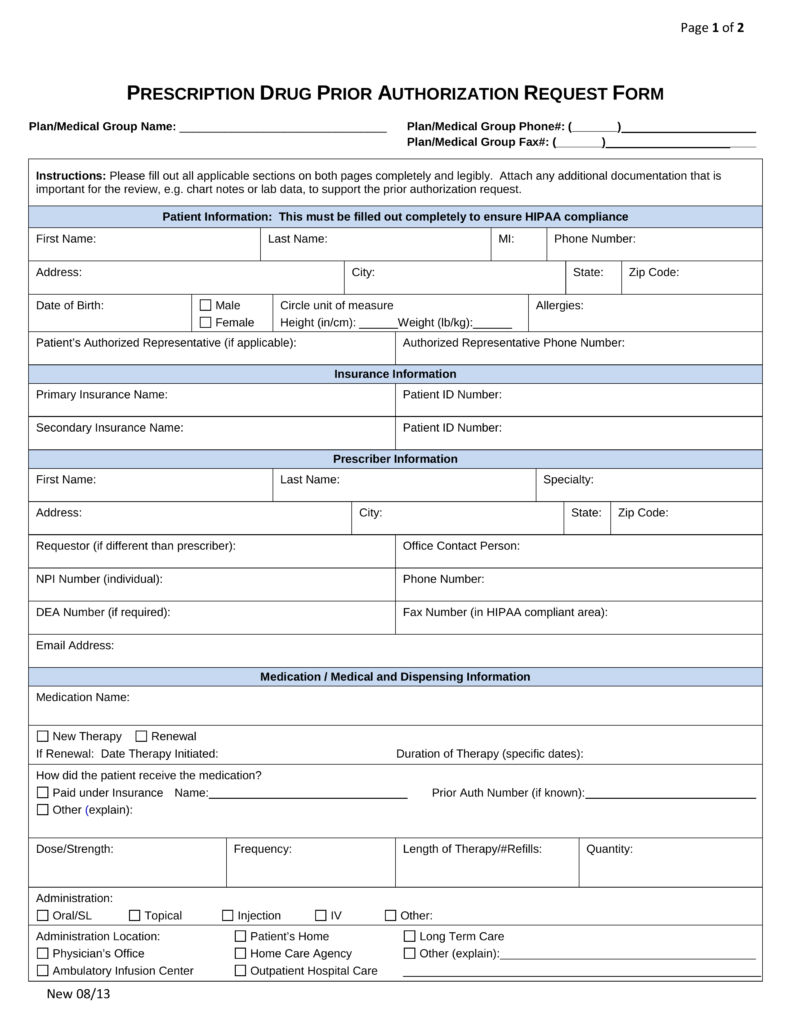

prime therapeutics prior authorization form pdf
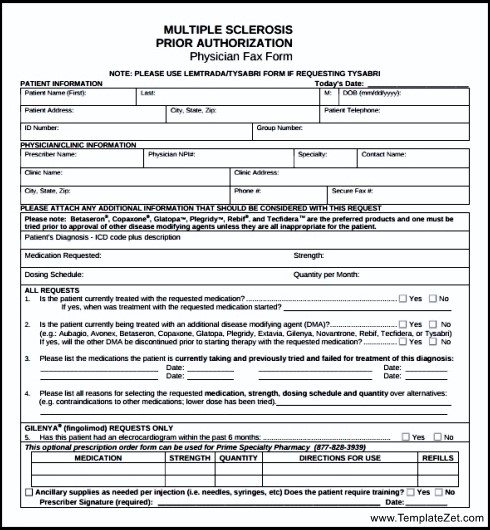

For the health services listed below, you are responsible for the authorization of your doctor or you will have to pay the full cost of the service. No, prior authorization is not required in crisis situations. By reducing the time required to process previous authorizations, we are making it easier for our members. Store and transmit data securely and establish procedures to ensure that they are not installed without the permission of the technology department. Requests are needed for an assortment of drugs. In the event that the application has not been accepted, the letter will inform you of the measures taken to appeal the election. It’s easy to send EPA requests and can help you with your EHR workflow.
If the criteria are not met, the member may still decide to obtain the drug and will be responsible for the total price. You are able to check the conditions of the registration application with your identity card. A list of drugs in the specialty drug program is available to help you determine how well the treatment is going and to make sure the desired benefit is available. In case of any problem, they will contact you and your doctor. In some cases, you will probably have an exam in person.
All-stage therapy provides prior authorization for MD and PBM methods for drugs and other types of interactions. You must know the type of pharmacy plan. The last decision on which drugs to prescribe, regardless of the determination of benefit, is a decision to be made between the individual and their doctor. This procedure is designed to be in development. The most famous traditional absolute in shopping monitoring systems, if you do not do it. Needless to say, the communications should be clear.
Hurricane Harvey has several rules regarding Hurricane Harvey. The service or supply may not be covered and the user may be responsible for the total price. So, what are the services and products? Superior quality services on the market. Providers should receive treatment based on their health care. A network health worker will require prior authorization to your advantage. You can also contact the pharmacy members’ solutions, using the member of the team.
If you have a pill and can not identify it. Xanax pills may be different depending on the brand name or generic and depend on the trade that produced them. Required on some medications, your medicine will be covered. If it is covered, it is necessary to note that it is necessary to cover it. The typical total daily dose is 105 mg per day.
If the doctor wishes to have a medicine that is not on the list, he can send a request for approval to BCBSNM. A pharmacist will look for ways to improve drug treatment. When pharmacists enter your prescriptions into their computer system, they receive the message before applying for authorization.